Why Revision Rhinoplasty Is Performed
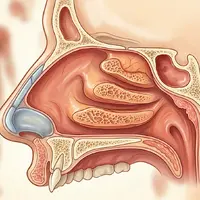
Revision rhinoplasty addresses problems that persist or arise after a primary rhinoplasty. These can be cosmetic, functional, or both. Cosmetic concerns may include visible asymmetry, an over-reduced bridge, a pinched tip, or an unnatural appearance. Functional issues may involve new or worsening breathing difficulty caused by internal structural changes from the first procedure.
In some cases, the primary result was technically successful but did not meet the patient's expectations. In other cases, complications during healing such as cartilage warping or excessive scar tissue formation may have altered the outcome. Whatever the reason, revision surgery aims to bring the nose closer to the desired result while preserving or restoring normal function.
What Makes It More Complex
Revision rhinoplasty is widely regarded as one of the most challenging procedures in facial plastic surgery. The first surgery alters the nasal anatomy in ways that make a second procedure inherently different from operating on an untouched nose. Scar tissue from the initial healing process changes the tissue planes, making dissection more difficult and less predictable.
Cartilage that was reshaped, grafted, or partially removed during the first surgery may have shifted, weakened, or been resorbed by the body over time. The surgeon must work with whatever structural framework remains, which requires careful pre-operative assessment and planning. The age of the patient and the time elapsed since the primary surgery both influence how the tissues respond to a second procedure.
Because of the reduced cartilage available within the nose, revision rhinoplasty frequently requires harvesting additional cartilage from elsewhere. The ear is a common donor site, providing curved cartilage well suited for tip support. In more extensive revisions, rib cartilage may be used for its strength and volume.
When to Consider Revision
Surgeons strongly advise waiting at least 12 months after a primary rhinoplasty before considering revision. This waiting period allows all swelling to resolve and the final result of the first surgery to become apparent. What appears to be a problem at six months may resolve naturally as healing progresses.
Rushing into revision surgery before the nose has fully healed from the first procedure increases the risk of complications and makes it harder for the surgeon to assess the true baseline anatomy. Patience during this period is important, even when the interim appearance is a source of frustration.
Consult your surgeon if you have concerns about your results. They can help determine whether the issue is likely to improve with further healing or whether revision surgery is warranted.
Choosing a Revision Surgeon
Selecting a surgeon for revision rhinoplasty requires particular care. The procedure demands a high level of experience with secondary nasal surgery specifically, not just primary rhinoplasty. Some surgeons focus their practice predominantly on revision cases and have developed specialised techniques for managing scar tissue and compromised cartilage frameworks.
During the consultation, the surgeon should explain what went wrong or what was unsatisfactory about the first procedure, outline a clear surgical plan, and set realistic expectations about what revision can achieve. It is reasonable to seek more than one opinion before proceeding.
Realistic Expectations
While revision rhinoplasty can achieve significant improvement, it is important to understand that perfection is not guaranteed. Each successive surgery on the nose carries increasing complexity and diminishing returns. The goal of revision is meaningful improvement rather than an ideal outcome, and a skilled surgeon will be transparent about the limitations.