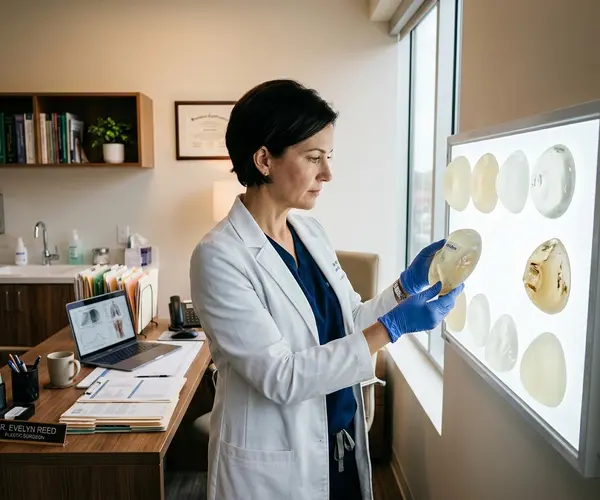
Why Implants Are Not Permanent
Breast augmentation delivers long-lasting results, but the implants themselves are medical devices with a finite lifespan. Both silicone gel and saline implants are manufactured to be durable, yet they are subject to wear over time. The shell can weaken, the fill material can change, and the body's own tissue response around the implant can evolve.
Manufacturers generally warrant their implants for 10 years, and clinical data supports the expectation that many implants function well for 10 to 20 years or longer. However, the absence of symptoms does not guarantee the implant is intact. This is why ongoing monitoring is a standard recommendation from both the FDA and major plastic surgery societies.
Rupture and How It Presents
Implant rupture is one of the main reasons patients undergo replacement surgery. The risk of rupture increases as the implant ages, though it can occur at any point.
With saline implants, a rupture is usually immediately obvious. The saline solution leaks out, the breast deflates noticeably, and the body absorbs the sterile saltwater without harm. The implant shell still needs to be removed and replaced.
Silicone gel ruptures are often "silent," meaning there may be no visible change in breast shape or size. The cohesive gel tends to stay within the implant shell or the surrounding scar tissue capsule rather than migrating. This is why the FDA recommends periodic MRI or ultrasound screening for silicone implants to detect silent rupture, typically starting five to six years after surgery and every two to three years thereafter.
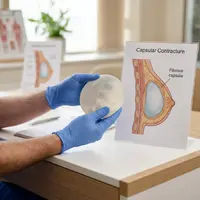
Capsular Contracture
The other major reason for implant replacement is capsular contracture. After any implant is placed, the body naturally forms a thin layer of scar tissue around it. In some cases this capsule tightens and hardens, squeezing the implant and causing firmness, discomfort, or visible distortion.
Capsular contracture can develop at any stage but is more common as years pass. Not all cases require surgery. Mild contracture (Baker grades I and II) may need only monitoring, while more severe cases (grades III and IV) typically require capsulectomy and implant replacement.
When to Consider Replacement
There is no fixed expiration date stamped on an implant. The decision to replace is based on clinical findings, symptoms, and patient preference rather than a calendar alone. Common triggers include the following.
- Confirmed or suspected rupture on imaging
- Progressive capsular contracture causing discomfort or shape change
- A desire to change implant size, shape, or type
- Asymmetry that has developed over time
- Changes in breast tissue after pregnancy, weight fluctuation, or ageing
Some patients choose to have their implants removed entirely without replacement, a procedure called explant. Others opt for a new set of implants at the same time.
Long-Term Monitoring
Regardless of how your implants feel or look, periodic check-ups are advisable. Your surgeon or doctor can assess implant integrity through physical examination, ultrasound, or MRI. Early detection of silent rupture or early-stage contracture allows for planned, elective revision rather than an emergency scenario.
If you are approaching the 10-year mark or beyond, consult your surgeon to discuss whether imaging or a replacement plan is appropriate for your situation.